Perspectives from Africa and Asia: Our impact on communities
One in eight people lives more than an hour from their local health centre, and one in six is more than two hours from a hospital. For those living in rural areas, distances are often even greater, and people face additional barriers to accessing the care they need, such as travel costs and the cost of the treatment itself.
We train people living within hard-to-reach and remote communities to diagnose and treat common diseases. Often the first point of contact many families will have when facing ill-health, community health workers are known and trusted by their communities and can provide advice and treatment at no cost. They are the first line of defense in ensuring those most vulnerable to disease, especially women, children, mobile and migrant communities, and those living in conflict-affected settings don’t become another statistic.
Collaborating with mobile, migrant and forest-going workers to tackle malaria
In Cambodia and Ethiopia, we are reaching mobile and migrant communities with essential malaria services in remote and forested areas. They have extremely limited access to regular healthcare and preventive tools due to their mobility and work, which means their risk of infection is high.
In Cambodia, under the Regional Artemisinin-resistance Initiative 4 Elimination project (RAI4E), funded by the Global Fund, we are working with a community network of locally recruited and well-trained mobile malaria workers (MMWs) to offer quality malaria services to remote, mobile and migrant populations across six northern provinces along the international border with Thailand, Laos and Vietnam. Thanks to MMWs’ knowledge of local population movements, we are rapidly identifying and treat remaining pockets of malaria cases and prevent cross-border re-introduction.

San’s story: A tailored approach to detecting the last malaria cases in Cambodia
“Before I was asked to become a mobile malaria worker, I did not know at all that malaria was transmitted by mosquito bites. Also, nobody else in my village knew about this. After I was selected, I received training at the Siem Pang Health Center. This was not easy at all. I didn’t know anything about malaria and the nurse used so many difficult words — words I had never ever heard before. I asked them to speak a bit slower and explain to me again and again.
Now, I know very well how to test and treat people. I also have to write down all the names in a book. And I even use a phone to register all people who have malaria. When I started, I found so many malaria cases, mainly Plasmodium falciparum.
I can smile. The tests of people in my community do not show malaria anymore as before. People have learned a lot and understand better about malaria. They also use the nets that we distribute to protect themselves. I am so thankful for the malaria project and the support from the Malaria Consortium team. It made me so brave and knowledgeable. I am so proud.”
Healthcare worker tests young child for malaria
Healthcare worker tests young child for malaria
Mobile malaria worker tests boy for malaria
Mobile malaria worker tests boy for malaria
Mobile malaria worker tests forest worker for malaria
Mobile malaria worker tests forest worker for malaria

PROJECT SPOTLIGHT
Sennay
In Ethiopia, Sennay is the first ever at-scale implementation project to target malaria services to the specific contextual needs of seasonal mobile workers. We are implementing Sennay with the Health, Development and Anti Malaria Association, with funding from Expertise France/L’Initiative.
“The Sennay project is a game-changer in our fight against malaria. By focusing on seasonal mobile workers…we are addressing a critical gap in malaria prevention and control. This initiative not only aims to reduce the malaria burden but also empowers these workers by involving them in shaping the solutions. We are creating sustainable health improvements and ensuring that no one is left behind in this critical fight.”
Extending primary health services in conflict and humanitarian settings
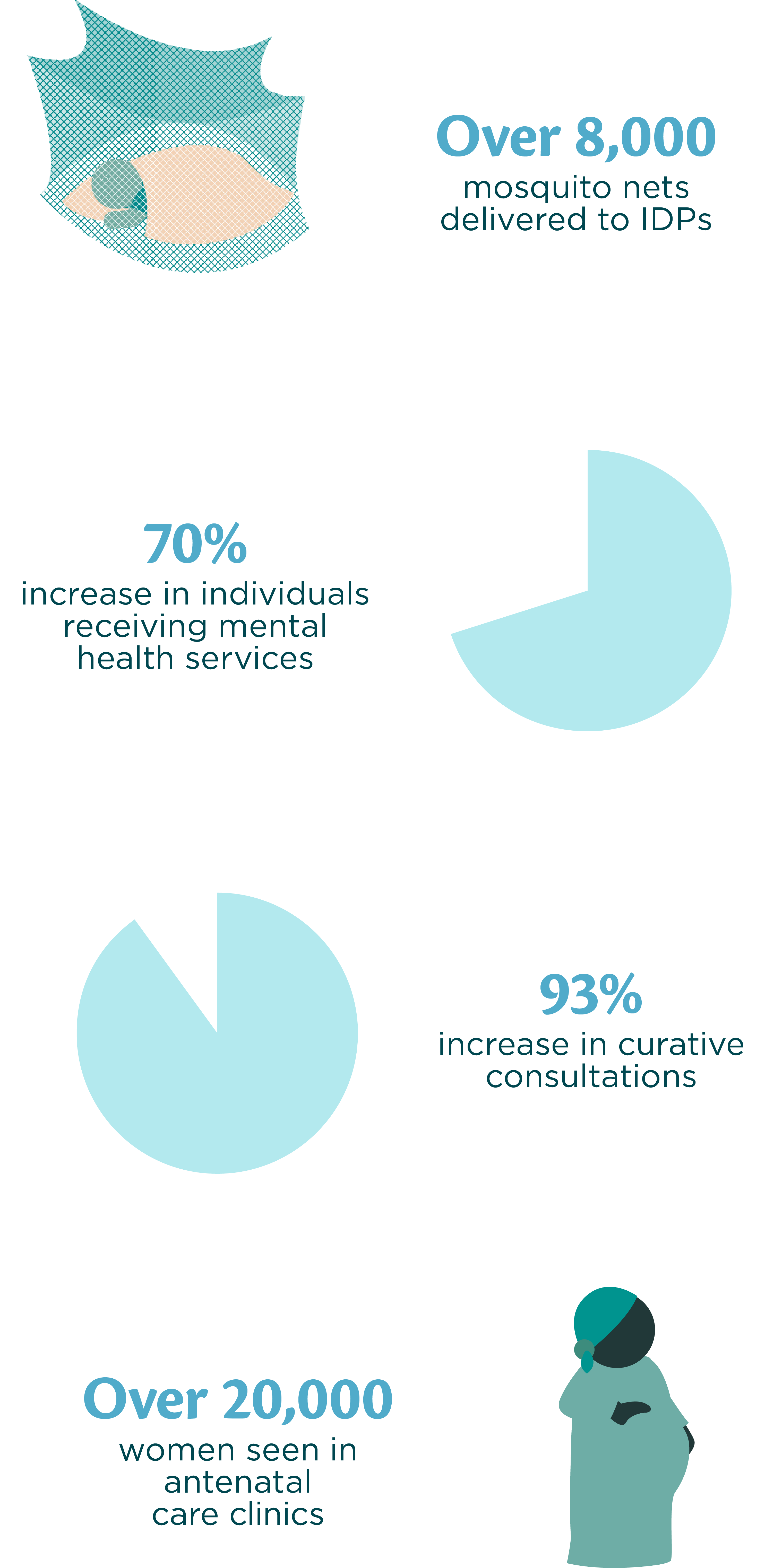
Everyone deserves access to quality healthcare. They shouldn’t be left behind simply because conflict, persecution, flooding due to extreme weather events, or food insecurity have forced them from their homes. We're providing life-saving primary healthcare to thousands of internally displaced people (IDPs), refugees and returnees, host communities and other at-risk populations with essential health services, through networks of trained local community health workers and alternative delivery methods, such as mobile clinics.
Reaching displaced communities in South Sudan
In South Sudan, an unprecedented humanitarian crisis arising from disruptions, including extreme weather events and conflict, has displaced more than two million people. More than half of the population also lives more than five kilometres from the nearest health facility.
Working with the Ministry of Health, the Health Pooled Fund and UNICEF, we have successfully expanded the coverage and delivery of community health services to remote and hard-to-reach communities through the Boma Health Initiative (BHI), with funding from UK Development and the Global Fund to Fight AIDS, Tuberculosis and Malaria. This seven-year nationwide community health programme has strengthened health services delivery to communities, with a particular focus on pregnant women and children. In 2023, we began co-developing a digital tool with the Ministry of Health to improve the collection, reporting and use of BHI data. This means we can more accurately and effectively target resources where the greatest needs are identified.

Implementing SMC in an IDP camp
We go the extra mile to ensure that no one is left behind. In 2023, South Sudan saw an influx of refugees from neighbouring Sudan, including 500 children living in an IDP camp in one of the SMC-implementing counties. We made several adaptations to the SMC delivery model to ensure that these children were able to receive life-saving antimalarial medicines being distributed as part of the SMC round.
Implemented stringent security measures and operational protocols during SMC delivery, we worked closely with the National Malaria Control Programme to engaged a wide array of stakeholders, including the United Nations High Commissioner for Refugees, camp management committees and the State Ministry of Health. Our team also established direct communication channels with local leaders from the refugee community.
Using this proactive approach, we were able to respond quickly to emerging issues, enhance community trust, and ensure the safety of staff and the refugee community alike.
Strengthening our commitment to women in marginalised and remote populations
HPV Catch-up to tackle cervical cancer in Cambodia
Despite being preventable and treatable, cervical cancer killed 350,000 women in 2022 and remains the fourth most common cancer in women worldwide, disproportionately affecting those in low- and middle-income countries. This means that women in communities at risk of malaria might also be at risk of cervical cancer. This disease can be prevented with effective vaccines that target its primary cause, human papilloma virus (HPV). If diagnosed early and managed effectively, it is also one of the most successfully treated forms of cancer.
In 2024, we launched a pioneering cervical cancer project in Thma Pouk district, Banteay Meanchey province in Cambodia — a region often overlooked for health services due to its remote location. Cambodia has one of the highest rates of cervical cancer disease and death in the world, despite being easily prevented and treated if detected early. More than 1,500 women develop cervical cancer each year in Cambodia as a result of lack of access to health services.
Community dialogue regarding human papilloma virus (HPV)
Community dialogue regarding human papilloma virus (HPV)
Programme Manager Ratanakvisal Chean shares his experience of meeting with the district officials during the project launch:
“When we met with district governors and the operational district, they asked a question that resonated deeply with me: ‘Are we the last district you targeted?" It was a poignant reminder of how often this community had been left behind.
One governor offered to personally assist with community engagement, highlighting the district's readiness to take action: 'If you need help with raising awareness on cervical cancer, I’m more than happy to join you in the villages and encourage participation.'
Another governor expressed her concern about the HPV Catch-up project ending in December 2024: 'Would you be able to extend the project here? Cervical cancer is such a crucial topic, and it has never been addressed in this district before.'
The experience in Thma Pouk district was a call to action, a shared commitment to ensuring that cervical cancer awareness and prevention reach every corner of Cambodia. With the support of the local leaders and the determination of our team, we are confident that this project will make a lasting impact, bringing much-needed change to a district that has long awaited its turn.”


Promoting sexual and reproductive health in South Sudan
In humanitarian and conflict settings, women and girls are at a greater risk of experiencing gender-based violence (GBV). Survivors of GBV are also more likely to experience mental health concerns and might also be living with a disability, often struggling to access the healthcare they need due to unstable conditions. Our expertise in delivering malaria services and community-based health services in South Sudan enables us to extend access to other vital services including for sexual and reproductive health, psychosocial support and disability.
To improve access to sexual health and reproductive services among women and girls, Malaria Consortium introduced a gender equality and social inclusion programme in Aweil Centre and Aweil South, Northen Bahr El Ghazal state as part of the Health Pooled Fund project. The programme trained healthcare workers on gender-based violence, clinical management of rape, mental health conditions, disability inclusion and adolescent sexual reproductive health rights.
We identified influential women and religious leaders to engage marginalised women and girls, like Adut, to become adolescent sexual and reproductive health rights champions.
4,558
community members reached with sexual and reproductive health messages
6,700
school students reached with health talks and debates
Adut, Adolescent Sexual and Reproductive Health Rights Champion, Northern Bahr el Ghazal, South Sudan
Adut, Adolescent Sexual and Reproductive Health Rights Champion, Northern Bahr el Ghazal, South Sudan
Adut's story
“I became involved with the project through discussions organised at the Sexual Reproductive Health Centre at Aweil Civil hospital.
“Because of this project, the stigma surrounding sexual health is slowly reducing. Girls, including young mothers, can come to the health centre to access essential services without fear. Sharing sexual and reproductive health information works especially well to reduce pregnancy rates within girls and adolescents in schools, as there are a high number of girls enrolled within local schools who are informed of the family planning commodities available at their nearest health facility.
“In the future, we hope to continue to increase the number of awareness sessions within the community, training community mobilisers and counsellors to…reach everyone.”