Our response
The adaptations we made to continue delivering interventions to the communities who depend on them
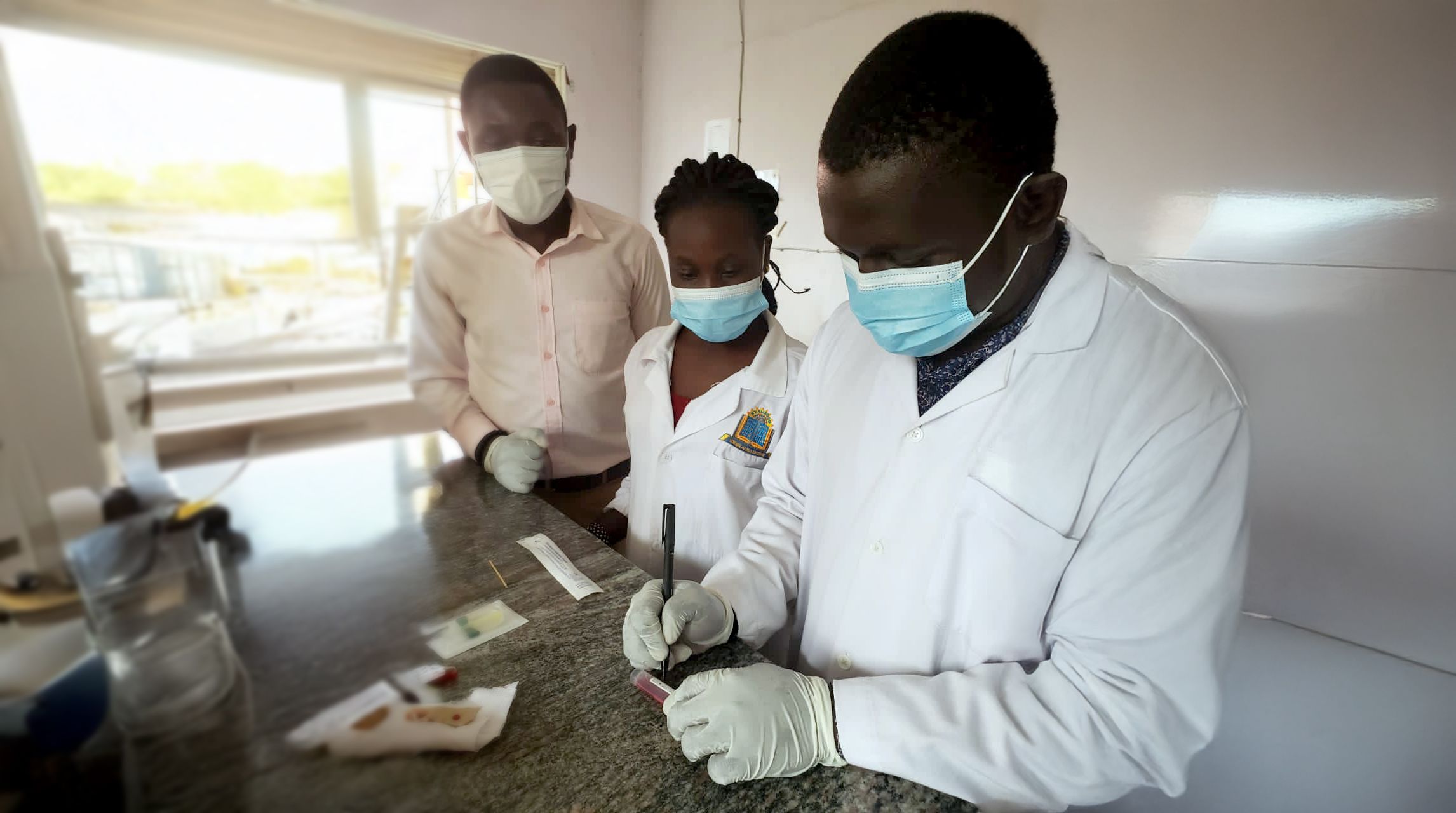
Through effective teamwork and adaptation, Malaria Consortium was able to continue delivering programmes throughout the COVID-19 pandemic with minimal delays, and without placing our staff and communities at undue risk.
Programmes such as seasonal malaria chemoprevention (SMC) require delivery on precise timescales, specifically before the rainy seasons, when malaria transmission peaks. The pandemic threatened to throw these delicate plans into chaos, with potentially disastrous consequences for the many lives that depend on them.
Malaria Consortium was able to continue to deliver crucial care to the communities with whom we work. Our proactive and evidence-based approach during the pandemic ensured that essential malaria services continued despite significant disruptions and uncertainty. Malaria prevention and control services in Nigeria were not only maintained, but actually increased in some cases.
The Uganda team evaluated the impact of the pandemic on essential malaria services in northern Uganda. National lockdown affected access to, and delivery of, essential malaria services. Malaria Consortium recommended that the Ministry of Health and district health departments should strengthen health education on malaria alongside education on COVID-19 prevention.
We helped to develop guidance for countries that advised on how to roll out SMC activities while still aligning with national COVID-19 responses. This ensured the safety of communities and health workers while maintaining essential malaria prevention efforts.
Our well-built systems meant that we could quickly pivot our efforts to address COVID-19. Malaria Consortium helped to lead on the distribution of crucial COVID vaccines in some of the regions where we work, such as South Sudan, and of personal protective equipment (PPE) to frontline health workers in Uganda. In other areas, operations were able to simply continue as usual, owing to the resilience of the systems that Malaria Consortium had put in place. In Cambodia, mobile malaria workers were already equipped with masks and gloves, as well as sanitisers, and didn’t have to contend with limited stock like so many others.
In Mozambique, the organisation adapted upSCALE, an existing digital health platform, to help community health workers respond to COVID-19 alongside case management for other diseases, including malaria and pneumonia.

Spotlight: Maintaining malaria services in Nigeria
When the first case of COVID-19 was reported in Nigeria on 27 February 2020, Malaria Consortium was already working in partnership with local and national governments in 11 states across the country. We were ideally placed to support the national malaria elimination programme overcome challenges presented by the pandemic and ensure malaria services continued.
"Malaria Consortium is playing a primary role in sustaining collaboration with other Roll Back Malaria partners in the national programme to ensure our efforts towards a malaria-free Nigeria are coordinated and harmonised as we address the COVID-19 pandemic and beyond.”
Lockdown measures included restrictions on travel and in-person meetings, which impacted on lines of communication between the National Malaria Elimination Programme and local partners, causing many malaria control activities to cease. Restrictions on the movement of malaria commodities led to stockouts, and many health facilities shut, which left people unable to access diagnostic and treatment services.
Our response
We re-established lines of communication by purchasing videoconferencing software licences for the national and state malaria elimination programmes in Lagos and Kano. Other partners followed our example, purchasing licences for other states.
We adapted guidance on outbreak response and continuity of malaria services to the Nigerian context, informing the NMEP’s Guidelines for Business Continuity in Emergency. By outlining new methods for campaign delivery, we were able to ensure staff safety.

Adapting LLIN campaigns
Providing health workers with a wheelbarrow to deliver nets door to door reduced contact between people from different households. This approach combined community mobilisation and distribution, reducing contact points between the health workers and community members. Delivering directly to households meant that health workers could show people how to use the nets in their own homes. These adaptations were effective and fostered equity.
Modifying SMC campaigns
We developed protocols for infection prevention and control — this included maintaining a distance of two metres, where possible, wearing PPE, and washing or sanitising hands between visits. The method of delivery was also modified: health workers showed someone in the household how to give the treatment from a safe distance, reducing physical contact. This approach was effective as children were often more relaxed when given treatment by someone in their household instead of by a community health worker.
Strengthening the capacity of community health workers
Recognising the importance of community health workers to communities who were unable to travel to health facilities for treatment, we incorporated guidance on infection prevention and control and reducing COVID-19 transmission risk into the community health workers’ guide for implementing integrated community case management. Community health workers also received training to deliver information on COVID-19 to communities.
Spotlight: Supporting health workers in Uganda
One of the biggest barriers to maintaining malaria services in Uganda at the start of the pandemic was fear, both among health workers and the general population. The overlap of symptoms between malaria and COVID-19 meant people with fever were afraid to seek treatment for fear of stigma and being put into isolation, and health workers didn’t want to come into contact with them. On top of this, lockdowns and social distancing disrupted access to healthcare and limited the availability of public transport.
Our response
Malaria Consortium is a long-term partner of the Ugandan Ministry of Health and had active projects in much of the country when the first case was confirmed on 21 March 2020. As a result, we were able to support the National Malaria Control Division develop context-appropriate guidelines and adapt programmes, ensuring activities went ahead.

Protocols for malaria testing and treatment
We advocated for all patients presenting with fever to be tested for malaria in the first instance before presuming a COVID-19 diagnosis.
As manufacturers pivoted to focus on COVID-19 diagnostic tests, stockouts of malaria tests began to occur. We advised that, where malaria diagnostics were not available, health workers should treat anyone presenting with fever for malaria in the first instance. After two days, if the patient had not responded to treatment, the health worker should consider an alternative condition.
Upskilling and protecting community health workers
We strengthened the capacity of
33,000 health workers
to safely diagnose and treat COVID-19
To reduce fear among health workers and protect them against COVID-19 transmission, Malaria Consortium implemented a project that trained 25 percent of Uganda’s village health teams on infection prevention and control measures, including use of PPE and handwashing. We secured approval to deliver supplies of masks, goggles, soap and hand sanitisers to 40 districts across the country. Alongside this, we sent out health communication over the radio to encourage people to seek prompt treatment if they had a fever.
Adapting service delivery and distribution campaigns
We supported health centres to rearrange their set-ups to allow for social distancing, including offering some services outside in the open air or in a tent under a tree.
As in Nigeria, we adapted mosquito net distribution campaigns to follow a door-to-door distribution approach, which avoids bringing groups of people together. Distributors used mobile phones to register households and record net distribution. Malaria Consortium staff switched to providing support remotely, online or via phone, to ensure support and supervision to health workers could be maintained and programmes continued.
Spotlight: Continuing delivery in Cambodia
Our long-established relationships with health authorities in Cambodia, coupled with existing infection prevention and control practices, ensured that malaria services could continue with minimal disruption during the COVID-19 pandemic. Malaria Consortium has worked with the National Center for Parasitology, Entomology and Malaria Control (CNM) for the past two decades to reduce malaria in Cambodia, ensuring the country is on track to elimination. The first case of COVID-19 was confirmed early on, on 27 January 2020. However, restrictions were rapidly put in place and cases didn’t start to rise rapidly until over a year later. We continued our work to support malaria services in six border provinces throughout the pandemic.

Our response
Stocks of commodities within provinces
With restrictions on movement between provinces in place, we faced logistical challenges in delivering some malaria commodities, such as hammock nets, which we distribute to forest workers to protect themselves when sleeping outside. However, malaria commodities for testing and treatment were well stocked within provinces so the travel restrictions didn’t affect case management. It was already standard practice to provide health workers with PPE and hand sanitisers.
Local recruitment of malaria workers
Lockdowns prevented the team in Phnom Penh from visiting the provinces to provide supervision and support to village and mobile malaria workers. However, because malaria workers are locally recruited, they were able to continue providing malaria services in their communities without disruption. Switching communications to online platforms proved difficult due to connectivity issues in more remote areas. Where online communications were not viable, teams continued to meet face to face, where possible, while following strict infection prevention and control measures. Supervision teams communicated with malaria workers over the phone.
Working with health authorities
With large numbers of Cambodian nationals returning to their homes from work in Thailand, the government set up quarantine camps along the border for migrants, to prevent them from carrying COVID-19 to their home provinces. NGOs working in those areas were ordered to stop operations. Our good relationship with the health authorities meant that we could successfully negotiate with them — when we explained how stopping our operations would cause malaria cases to rise, we were permitted to continue our work with communities.
Adapted service delivery
We were unable to continue community dialogues due to restrictions preventing large gatherings, so we switched to a door-to-door approach with malaria workers delivering health messages to individual households. Although this approach was more time consuming, there was no drop-off in testing and delivery of services. Health workers normally visit health centres for a monthly meeting to report data and collect malaria commodities. To reduce contact between health workers, visits were staggered and any meetings were held outside, with social distancing rules observed.

