Reflections on the
COVID-19 pandemic
Five years of response, adaptation and impact
It is five years since the first signs of an impending pandemic began to emerge. To mark this milestone, Malaria Consortium reflects on lessons from this challenging time, from our perspective as a global health organisation dedicated to combating infectious diseases and ensuring the continued delivery of essential services to communities who need them most.
When reports of a new virus emerged in late 2019, we knew the risks — especially for sub-Saharan Africa, where health systems are already stretched by infectious diseases like malaria. By the time the World Health Organization (WHO) predicted that disruptions to malaria prevention and control services could double deaths from malaria, Malaria Consortium was already launching a response to limit disruption to the malaria programmes we support.
As COVID-19 spread, we acted fast, working with partners to protect malaria and other health programmes, and prevent the devastating impact WHO had warned about.
This timeline charts how we adapted, the challenges we faced and what we learned along the way. It also sets out urgent steps — both for us and the global community — to ensure we’re ready for future health crises.
DECEMBER 2019
A novel coronavirus is detected in Wuhan province, China
“Within two weeks or so we went from ‘that's something we need to watch’ to ‘this is going to change everything.’”
Public health staff at Malaria Consortium are closely following the reports of cases of pneumonia with unknown cause.

A novel coronavirus is detected in Wuhan province, China
“Within two weeks or so we went from ‘that's something we need to watch’ to ‘this is going to change everything.'”
Public health staff at Malaria Consortium are closely following the reports of cases of pneumonia with unknown cause.

JANUARY 2020
Cases start to spread beyond China's borders and the first deaths are reported.
Concerns are growing within the organisation. Staff with experience of managing outbreaks and supporting countries to develop pandemic preparedness plans start to see the warning signs associated with a pandemic.
"Suddenly I realised that this is something really serious... We have no answers and need to be doing something about it. That's when my mindset really changed because I realised that there's something horribly wrong going on and we need to be prepared for it.”
30 JANUARY 2020
19 countries have reported cases of COVID-19.
The WHO declares COVID-19 a public health emergency of international concern.
Image: WHO COVID official visit of the UN Secretary-General


Cases start to spread beyond China's borders and the first deaths are reported.
Concerns are growing within the organisation. Staff with experience of managing outbreaks and supporting countries to develop pandemic preparedness plans start to see the warning signs associated with a pandemic.
"Suddenly I realised that this is something really serious... We have no answers and need to be doing something about it. That's when my mindset really changed because I realised that there's something horribly wrong going on and we need to be prepared for it.”
30 JANUARY 2020
Credit: UN Geneva | Flickr
Credit: UN Geneva | Flickr
19 countries have reported cases of COVID-19.
The WHO declares COVID-19 a public health emergency of international concern.
Image: WHO COVID official visit of the UN Secretary-General

FEBRUARY 2020
Malaria Consortium begins talks with the WHO to discuss concerns about the resilience of health systems in sub-Saharan Africa, and the impact this could have on the delivery of malaria services if COVID-19 spreads to the region.
“One of the things I stressed is that if we have a pandemic and we have weak health systems where we are working this is a time when our communities actually need more of us. We decided that it was not about closing down our delivery... but it was looking at how we then shift to virtual remote working and ramp up our activities."
27 FEBRUARY 2020
The first case of COVID-19 is confirmed in sub-Saharan Africa, in Nigeria.
Maintaining malaria services in Nigeria
Malaria Consortium has worked with with the National Malaria Elimination Programme (NMEP) in Nigeria for over 15 years. During the COVID-19 pandemic, we supported the NMEP to develop and implement guidelines to maintain malaria services. Some of the modifications made to long-lasting insecticide-treated nets and seasonal malaria chemoprevention campaign strategies resulted in more effective implementation than the existing strategy, and have since become part of our core delivery strategies. The pandemic also highlighted the importance of community health workers during emergencies.
Image: Community-directed distributor, Nigeria

Malaria Consortium begins talks with the WHO to discuss concerns about the resilience of health systems in sub-Saharan Africa, and the impact this could have on the delivery of malaria services if COVID-19 spreads to the region.
“One of the things I stressed is that if we have a pandemic and we have weak health systems where we are working this is a time when our communities actually need more of us. We decided that it was not about closing down our delivery... but it was looking at how we then shift to virtual remote working and ramp up our activities."
Credit: Light Oriye
Credit: Light Oriye
27 FEBRUARY 2020
The first case of COVID-19 is confirmed in sub-Saharan Africa, in Nigeria.
Maintaining malaria services in Nigeria
Malaria Consortium has worked with with the National Malaria Elimination Programme (NMEP) in Nigeria for over 15 years. During the COVID-19 pandemic, we supported the NMEP to develop and implement guidelines to maintain malaria services. Some of the modifications made to long-lasting insecticide-treated nets and seasonal malaria chemoprevention campaign strategies resulted in more effective implementation than the existing strategy, and have since become part of our core delivery strategies. The pandemic also highlighted the importance of community health workers during emergencies.
Image: Community-directed distributor, Nigeria
MARCH 2020
COVID-19 cases have been confirmed in 114 countries. The WHO officially declares COVID-19 a pandemic.
Protecting community health workers in Uganda
When the first case of COVID-19 was confirmed in Uganda, on 21 March 2020, the country was already grappling with an Ebola outbreak. With active projects across Uganda, we were well-placed to support the Ministry of Health to maintain essential malaria services during the pandemic. Malaria Consortium trained village health workers in infection prevention and control and procured personal protective equipment for them — delivering masks, goggles, soap and sanitisers to 40 districts across the country. In addition, we implemented health communication through radio messages that encouraged people to seek treatment promptly if they had a fever.
21 MARCH 2020
Malaria Consortium closes the office in London and staff are supported to work from home.
23 MARCH 2020
The UK Government issues a nationwide stay-at-home order.
In late March, the WHO issued a statement urging countries to ensure the continuity of malaria services and publishes interim operational guidance for maintaining essential health services during an outbreak.
Image: Village health team member, Uganda


COVID-19 cases have been confirmed in 114 countries. The WHO officially declares COVID-19 a pandemic.
Protecting community health workers in Uganda
When the first case of COVID-19 was confirmed in Uganda, on 21 March 2020, the country was already grappling with an Ebola outbreak. With active projects across Uganda, we were well-placed to support the Ministry of Health to maintain essential malaria services during the pandemic. Malaria Consortium trained village health workers in infection prevention and control and procured personal protective equipment for them — delivering masks, goggles, soap and sanitisers to 40 districts across the country. In addition, we implemented health communication through radio messages that encouraged people to seek treatment promptly if they had a fever.
21 MARCH 2020
Malaria Consortium closes the office in London and staff are supported to work from home.
Village health team member, Uganda. Credit: Light Oriye
Village health team member, Uganda. Credit: Light Oriye
23 MARCH 2020
The UK Government issues a nationwide stay-at-home order.
In late March, the WHO issued a statement urging countries to ensure the continuity of malaria services and publishes interim operational guidance for maintaining essential health services during an outbreak.
Image: Village health team member, Uganda
APRIL 2020
The WHO warns that severe disruptions to insecticide-treated net campaigns and access to antimalarial medicines could double deaths in sub-Saharan Africa.
4 APRIL 2020
Over 1 million cases of COVID-19 are confirmed worldwide.
With the rainy season approaching in many countries, any delays in decision-making will result in lives lost. Malaria Consortium sets out to lead a response and make decisions based on the broad expertise and knowledge of the global team. Staff start adapting campaigns to ensure they can be delivered safely while adhering to the COVID-19 restrictions in each country.
“The overarching priority was we need to do what we can to keep things going.”
“[We asked]how do we deliver what we do safely, rather than should we deliver it.”
Throughout the COVID-19 pandemic, Malaria Consortium is guided by the principles of staff safety and continues to deliver life-saving services. While COVID-19 comes with a lot of uncertainty, the threat from malaria is certain if programmes don’t continue.

The WHO warns that severe disruptions to insecticide-treated net campaigns and access to antimalarial medicines could double deaths in sub-Saharan Africa.
4 APRIL 2020
Over 1 million cases of COVID-19 are confirmed worldwide.
With the rainy season approaching in many countries, any delays in decision-making will result in lives lost. Malaria Consortium sets out to lead a response and make decisions based on the broad expertise and knowledge of the global team. Staff start adapting campaigns to ensure they can be delivered safely while adhering to the COVID-19 restrictions in each country.
“The overarching priority was we need to do what we can to keep things going.”
“[We asked]how do we deliver what we do safely, rather than should we deliver it.”
Throughout the COVID-19 pandemic, Malaria Consortium is guided by the principles of staff safety and continues to deliver life-saving services. While COVID-19 comes with a lot of uncertainty, the threat from malaria is certain if programmes don’t continue.

MAY 2020
Malaria Consortium contributes to guidelines designed to support malaria surveillance, monitoring and evaluation in the face of faltering data collection due to COVID-19 restrictions imposed in several countries. The guidelines help address how existing data from routine health information systems can be interpreted to build a picture of the continuity of malaria services during the pandemic.
18-19 MAY 2020
The 73rd World Health Assembly, the first ever to be held virtually, adopted a landmark resolution to bring the world together to fight the COVID-19 pandemic.
Malaria Consortium's country teams support and advise governments to strengthen community health systems. Governments are focused on getting PPE to hospitals and health facilities. Malaria Consortium works hard to ensure that community health workers have the necessary PPE, where possible, to protect them while delivering services to families unable to travel due to lockdowns and transport disruptions.
“We advised that we strengthened the community health workers because they are closer to the community… so we then had to look for PPE to support our village health teams, that kept the services going.”
Continuation of services in Cambodia
In Cambodia, malaria services were able to continue relatively unhindered during COVID-19 and service utilisation actually increased during 2020. At the start of the pandemic, Malaria Consortium conducted a COVID-19 risk assessment and quickly developed and implemented a mitigation plan to ensure mobile malaria workers were able to continue providing malaria services without putting themselves or their patients at risk. Proactive programme planning, ongoing data monitoring and active engagement with communities and the national authorities circumvented the impact of COVID-19 on intervention coverage.
Faced with stockpiling of PPE across the globe, Malaria Consortium's global operations team comes up with creative solutions to secure and transport PPE across borders. This means we can ensure that all staff in the countries in which we work can carry out their activities safely.
Images: Community-directed distributor during door-to-door distribution of seasonal malaria chemoprevention, Nigeria
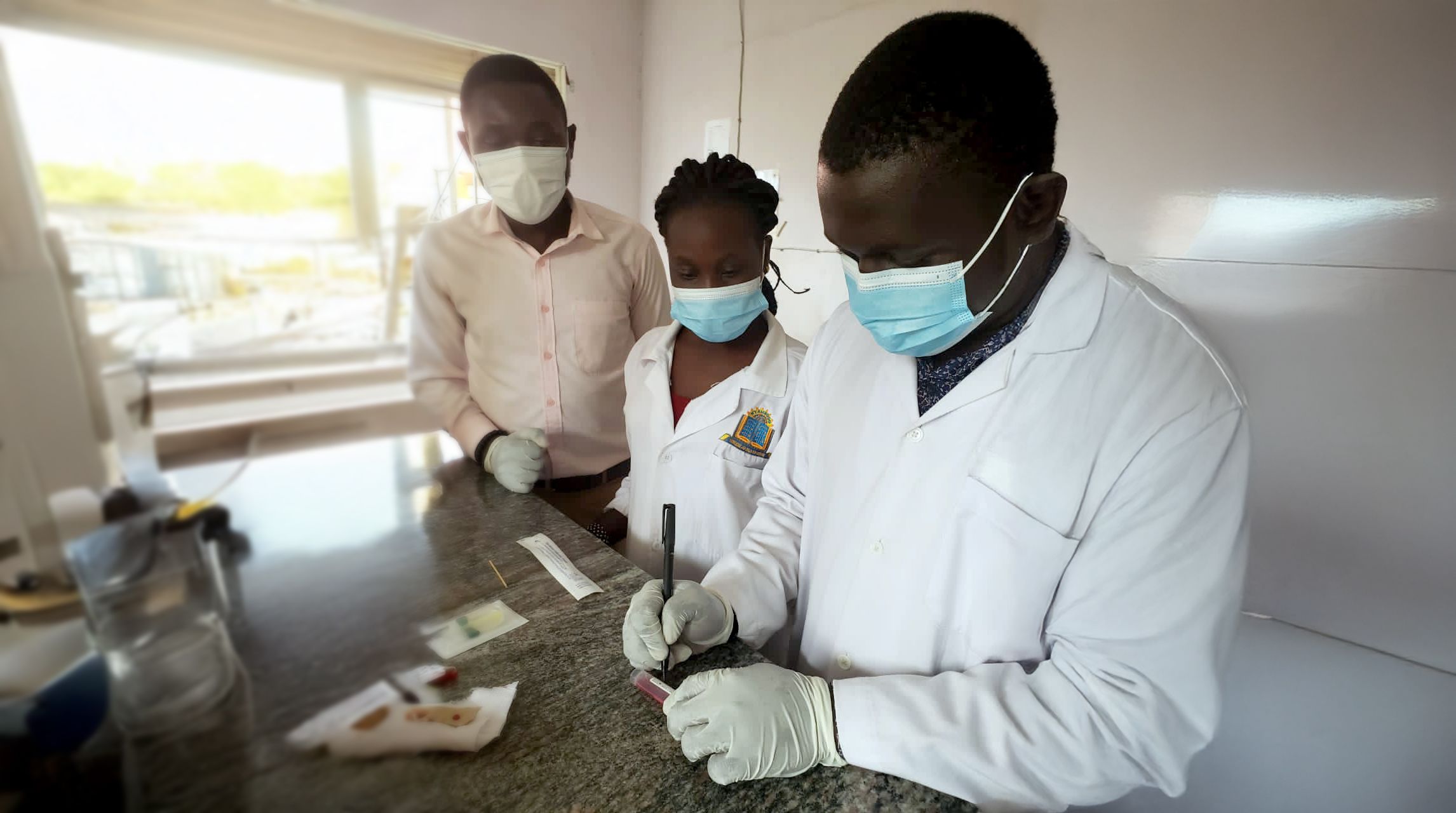
Malaria testing, Cambodia


Malaria Consortium contributes to guidelines designed to support malaria surveillance, monitoring and evaluation in the face of faltering data collection due to COVID-19 restrictions imposed in several countries. The guidelines help address how existing data from routine health information systems can be interpreted to build a picture of the continuity of malaria services during the pandemic.
Community-directed distributor during door-to-door distribution of seasonal malaria chemoprevention, Nigeria Malaria testing, Cambodia
Community-directed distributor during door-to-door distribution of seasonal malaria chemoprevention, Nigeria Malaria testing, Cambodia
18-19 MAY 2020
The 73rd World Health Assembly, the first ever to be held virtually, adopted a landmark resolution to bring the world together to fight the COVID-19 pandemic.
Malaria Consortium's country teams support and advise governments to strengthen community health systems. Governments are focused on getting PPE to hospitals and health facilities. Malaria Consortium works hard to ensure that community health workers have the necessary PPE, where possible, to protect them while delivering services to families unable to travel due to lockdowns and transport disruptions.
“We advised that we strengthened the community health workers because they are closer to the community… so we then had to look for PPE to support our village health teams, that kept the services going.”
Malaria testing, Cambodia
Malaria testing, Cambodia
Continuation of services in Cambodia
In Cambodia, malaria services were able to continue relatively unhindered during COVID-19 and service utilisation actually increased during 2020. At the start of the pandemic, Malaria Consortium conducted a COVID-19 risk assessment and quickly developed and implemented a mitigation plan to ensure mobile malaria workers were able to continue providing malaria services without putting themselves or their patients at risk. Proactive programme planning, ongoing data monitoring and active engagement with communities and the national authorities circumvented the impact of COVID-19 on intervention coverage.
Faced with stockpiling of PPE across the globe, Malaria Consortium's global operations team comes up with creative solutions to secure and transport PPE across borders. This means we can ensure that all staff in the countries in which we work can carry out their activities safely.
JUNE 2020
Malaria Consortium adapts the upSCALE digital health platform to send messages to community health workers and raise awareness of COVID among the population.
Malaria Consortium delivers COVID-19 messaging to communities by integrating it into existing projects wherever possible. This agile approach allows teams to send information on malaria and COVID-19 simultaneously without incurring any additional costs.
Adapting mosquito net campaigns
Following the successful modification of seasonal malaria chemoprevention campaigns, Malaria Consortium explored how best to continue to safely distribute mosquito nets without increasing transmission risk. We modified campaigns from using fixed collection points, where people typically gathered to collect their nets, to a door-to-door approach with nets delivered directly to households. Delivery teams wore appropriate PPE and observed social distancing, ensuring that contact was prevented between people from different families while also ensuring workers weren’t put at risk.

Malaria Consortium adapts the upSCALE digital health platform to send messages to community health workers and raise awareness of COVID among the population.
Malaria Consortium delivers COVID-19 messaging to communities by integrating it into existing projects wherever possible. This agile approach allows teams to send information on malaria and COVID-19 simultaneously without incurring any additional costs.
Adapting mosquito net campaigns
Following the successful modification of seasonal malaria chemoprevention campaigns, Malaria Consortium explored how best to continue to safely distribute mosquito nets without increasing transmission risk. We modified campaigns from using fixed collection points, where people typically gathered to collect their nets, to a door-to-door approach with nets delivered directly to households. Delivery teams wore appropriate PPE and observed social distancing, ensuring that contact was prevented between people from different families while also ensuring workers weren’t put at risk.
23 SEPTEMBER 2020
The 31st Meeting of the Roll Back Malaria (RBM) Partnership Surveillance, Monitoring, and Evaluation Reference Group (SMERG) provides an opportunity to exchange lessons learnt with key partners and stakeholders.
“Strong surveillance is the foundation for robust health systems. The COVID-19 pandemic brings with it risks of a diversion of resources and a drop in surveillance for other diseases like malaria. It is critical, at this time, to listen to a breadth of perspectives from different countries to reflect on our experience and lessons learnt. Collectively we’ll be able to better identify priorities, document best practice and identify optimal approaches that address both new and existing surveillance challenges.”
28 SEPTEMBER 2020
The WHO joins with partners to make 120 million affordable, quality COVID rapid tests available to low- and middle-income countries.
14-18 DECEMBER 2020
UK and South Africa report new SARS-CoV-2 variants to the WHO.
30 DECEMBER 2020
The WHO issues its first emergency use validation for a COVID-19 vaccine and emphasises the need for equitable global access.
Image: Community health workers in Mozambique show the upSCALE application on their mobile phones

Community health workers in Mozambique show the upSCALE application on their mobile phones
Community health workers in Mozambique show the upSCALE application on their mobile phones
23 SEPTEMBER 2020
The 31st Meeting of the Roll Back Malaria (RBM) Partnership Surveillance, Monitoring, and Evaluation Reference Group (SMERG) provides an opportunity to exchange lessons learnt with key partners and stakeholders.
“Strong surveillance is the foundation for robust health systems. The COVID-19 pandemic brings with it risks of a diversion of resources and a drop in surveillance for other diseases like malaria. It is critical, at this time, to listen to a breadth of perspectives from different countries to reflect on our experience and lessons learnt. Collectively we’ll be able to better identify priorities, document best practice and identify optimal approaches that address both new and existing surveillance challenges.”
28 SEPTEMBER 2020
The WHO joins with partners to make 120 million affordable, quality COVID rapid tests available to low- and middle-income countries.
14-18 DECEMBER 2020
UK and South Africa report new SARS-CoV-2 variants to the WHO.
30 DECEMBER 2020
The WHO issues its first emergency use validation for a COVID-19 vaccine and emphasises the need for equitable global access.
COVID-19 taskforce: Rapid response to changing risks
Seeing the rapid spread of the disease, Malaria Consortium staff set up a dedicated COVID-19 taskforce, made up of colleagues with experience in preventing and managing disease outbreaks. The group built a picture of the disease to understand how and where it was spreading and who was most at risk, gathering information from networks, peer-review publications, online resources and anecdotal evidence from country teams. The taskforce met regularly to analyse and discuss new information.
“I don't think there was a single decision that was made by any one individual it was continual debate, discussion, that got us to every single decision.”
Malaria Consortium started developing protocols to support staff to keep services running in the safest way possible. A global outbreak management plan was devised to help guide decision-making, with four risk categories defining our response within individual countries:
Each day the COVID-19 taskforce reviewed new data to determine if any countries had reached the threshold to move from one risk classification to another. These data included case counts, hospitalisations and deaths — and later vaccination rates — for each of the countries where Malaria Consortium operates.

24 FEBRUARY 2021
Ghana becomes the first country outside India to receive COVID-19 vaccine doses.
MARCH 2021
South Sudan receives its first supply of COVID-19 vaccine.
Uptake of COVID-19 vaccination in South Sudan is initially slow, with inadequate operational funding along with rising conflict and flooding hampering access to healthcare among hard-to-reach communities. Malaria Consortium implements the COVID-19 vaccination programme in the districts covered by our Health Pooled Fund project. To reach the WHO goal of 70 percent coverage by mid-2022, Malaria Consortium conducts a seven-day vaccination campaign in Aweil South to promote vaccination efforts and encourage community uptake.
7 APRIL 2021
So far, more than 38 million doses of COVID-19 vaccines have been delivered to over 100 economies across six continents.
12 MAY 2021
The Independent Panel for Pandemic Preparedness and Response (IPPPR) publishes its main report, with findings and recommendations for action to curb the COVID-19 pandemic and protect against future infectious disease outbreaks.
JUNE 2021
At the G7 Summit, dose-sharing commitments for 870 million additional vaccine doses are announced to support equitable access to vaccines in 2021 and 2022.
As vaccination rates increase and deaths from COVID-19 decrease, the organisation starts to re-open, allowing staff to return to offices, gather for meetings and resume international travel. We adopt a conservative, risk-based approach, on a country-by-country basis.
When reopening, offices continue to be equipped with masks and hand sanitisers, seating is spaced to allow for distancing, and the frequency of cleaning is increased. A protocol is also developed for notifying staff if someone has tested positive after recently visiting the office.
4 AUGUST 2021
The WHO calls for a moratorium on boosters until at least the end of September, to enable at least 10 percent of the population of every country to be vaccinated.
OCTOBER 2021
In a preliminary investigation to characterise COVID-19 cases in a high malaria burden setting, Malaria Consortium found that low previous malaria exposure seemed to be associated with more severe manifestations of COVID-19.
“Given the prevalence of malaria in sub-Saharan Africa, understanding the interactions and what this means for patient outcomes is of huge importance, and could help promote integrated approaches to investigations and management."
26 NOVEMBER 2021
The WHO designates Omicron a variant of concern.
During 2021, despite COVID-related challenges, Malaria Consortium managed to scale up the SMC programme, reaching 20 million children compared with six million reached in 2019.
“We got to 20 million children during a pandemic in the rainy season… so that for sure was by far the most important thing and the best thing that we could have done as an organisation.”
“The biggest success was we managed to implement without any major delays or disruptions and it also served as an example for other types of interventions.”
Image: Malaria vaccine rollout, South Sudan

24 FEBRUARY 2021
Ghana becomes the first country outside India to receive COVID-19 vaccine doses.
MARCH 2021
South Sudan receives its first supply of COVID-19 vaccine.
Uptake of COVID-19 vaccination in South Sudan is initially slow, with inadequate operational funding along with rising conflict and flooding hampering access to healthcare among hard-to-reach communities. Malaria Consortium implements the COVID-19 vaccination programme in the districts covered by our Health Pooled Fund project. To reach the WHO goal of 70 percent coverage by mid-2022, Malaria Consortium conducts a seven-day vaccination campaign in Aweil South to promote vaccination efforts and encourage community uptake.
Malaria vaccine rollout, South Sudan
Malaria vaccine rollout, South Sudan
7 APRIL 2021
So far, more than 38 million doses of COVID-19 vaccines have been delivered to over 100 economies across six continents.
12 MAY 2021
The Independent Panel for Pandemic Preparedness and Response (IPPPR) publishes its main report, with findings and recommendations for action to curb the COVID-19 pandemic and protect against future infectious disease outbreaks.
JUNE 2021
At the G7 Summit, dose-sharing commitments for 870 million additional vaccine doses are announced to support equitable access to vaccines in 2021 and 2022.
As vaccination rates increase and deaths from COVID-19 decrease, the organisation starts to re-open, allowing staff to return to offices, gather for meetings and resume international travel. We adopt a conservative, risk-based approach, on a country-by-country basis.
When reopening, offices continue to be equipped with masks and hand sanitisers, seating is spaced to allow for distancing, and the frequency of cleaning is increased. A protocol is also developed for notifying staff if someone has tested positive after recently visiting the office.
4 AUGUST 2021
The WHO calls for a moratorium on boosters until at least the end of September, to enable at least 10 percent of the population of every country to be vaccinated.
OCTOBER 2021
In a preliminary investigation to characterise COVID-19 cases in a high malaria burden setting, Malaria Consortium found that low previous malaria exposure seemed to be associated with more severe manifestations of COVID-19.
“Given the prevalence of malaria in sub-Saharan Africa, understanding the interactions and what this means for patient outcomes is of huge importance, and could help promote integrated approaches to investigations and management."
26 NOVEMBER 2021
The WHO designates Omicron a variant of concern.
During 2021, despite COVID-related challenges, Malaria Consortium managed to scale up the SMC programme, reaching 20 million children compared with six million reached in 2019.
“We got to 20 million children during a pandemic in the rainy season… so that for sure was by far the most important thing and the best thing that we could have done as an organisation.”
“The biggest success was we managed to implement without any major delays or disruptions and it also served as an example for other types of interventions.”
Image: Malaria vaccine rollout, South Sudan
Seasonal malaria chemoprevention: Overcoming barriers to implementation
Training for the seasonal malaria chemoprevention programme was due to start in April 2020, so the team had to act quickly to adapt protocols so the programme could start on time.
“We had a moral duty to try and do everything we could to continue to implement SMC as an essential malaria service, the rationale being that health systems were going to be disrupted and overburdened with COVID-19. If we then remove this essential health service, that's just going to add to the burden.”
Many caregivers found it challenging to adapt how antimalarial medicines are typically administered, to minimise physical contact between distributors and children. We explored the Role Model approach to address the issues associated with administration of SMC medication in Burkina Faso, Chad and Togo, and to find existing, local solutions.
The guidance we developed for the SMC campaigns demonstrated that continuing malaria services was possible. This became the blueprint for the safe delivery of other malaria interventions both within the organisation and globally.
“The WHO then took our standards and adapted them and then applied them globally, so we influenced the shape of the WHO's response, which then got applied to other interventions.”
Community health worker provides information to caregiver on seasonal malaria chemoprevention and COVID-19 prevention
Community health worker provides information to caregiver on seasonal malaria chemoprevention and COVID-19 prevention

15 JANUARY 2022
COVAX delivers its billionth COVID-19 vaccine dose, with a shipment of 1.1 million doses to Rwanda.
By March 2022, Malaria Consortium's vaccination campaign in Bahr el Ghazal state, South Sudan, has reached close to 27,000 people. WHO identified this as the highest COVID-19 vaccination rate across all ten states, with 11 percent of the state’s population fully vaccinated — more than double the national average.
APRIL 2022
Laboratory technicians centrifuge blood samples to separate plasma, Wolaita Sodo Referral Hospital, Ethiopia
Laboratory technicians centrifuge blood samples to separate plasma, Wolaita Sodo Referral Hospital, Ethiopia
Malaria Consortium begins a pioneering study in Ethiopia and Uganda that explores the relationship between cases of long COVID and malaria infections. The study goes on to find no increased prevalence of malaria infection after SARS-CoV-2 infection.

15 JANUARY 2022
COVAX delivers its billionth COVID-19 vaccine dose, with a shipment of 1.1 million doses to Rwanda.
By March 2022, Malaria Consortium's vaccination campaign in Bahr el Ghazal state, South Sudan, has reached close to 27,000 people. WHO identified this as the highest COVID-19 vaccination rate across all ten states, with 11 percent of the state’s population fully vaccinated — more than double the national average.
APRIL 2022
Laboratory technicians centrifuge blood samples to separate plasma, Wolaita Sodo Referral Hospital, Ethiopia
Laboratory technicians centrifuge blood samples to separate plasma, Wolaita Sodo Referral Hospital, Ethiopia
Malaria Consortium begins a pioneering study in Ethiopia and Uganda that explores the relationship between cases of long COVID and malaria infections. The study goes on to find no increased prevalence of malaria infection after SARS-CoV-2 infection.
5 MAY 2023
The WHO declares that COVID-19 no longer represents a global health emergency.
Dr Tedros Adhanom Ghebreyesus, head of the WHO, reveals that at least seven million people died in the pandemic, but the true figure is "likely" closer to 20 million deaths — nearly three times the official estimate.
The US and UK, like many other countries, have already talked about "living with the virus" and wound down many of the tests and social mixing rules.
By 14 April 2024, COVID-19 has caused an estimated 704,753,890 cases and 7,010,681 deaths globally.
"We fully expect that this virus will continue to transmit and this is the history of pandemics... It took decades for the final throes of the pandemic virus of 1918 to disappear. In most cases, pandemics truly end when the next pandemic begins."

5 MAY 2023
The WHO declares that COVID-19 no longer represents a global health emergency.
Dr Tedros Adhanom Ghebreyesus, head of the WHO, reveals that at least seven million people died in the pandemic, but the true figure is "likely" closer to 20 million deaths — nearly three times the official estimate.
The US and UK, like many other countries, have already talked about "living with the virus" and wound down many of the tests and social mixing rules.
By 14 April 2024, COVID-19 has caused an estimated 704,753,890 cases and 7,010,681 deaths globally.
"We fully expect that this virus will continue to transmit and this is the history of pandemics... It took decades for the final throes of the pandemic virus of 1918 to disappear. In most cases, pandemics truly end when the next pandemic begins."